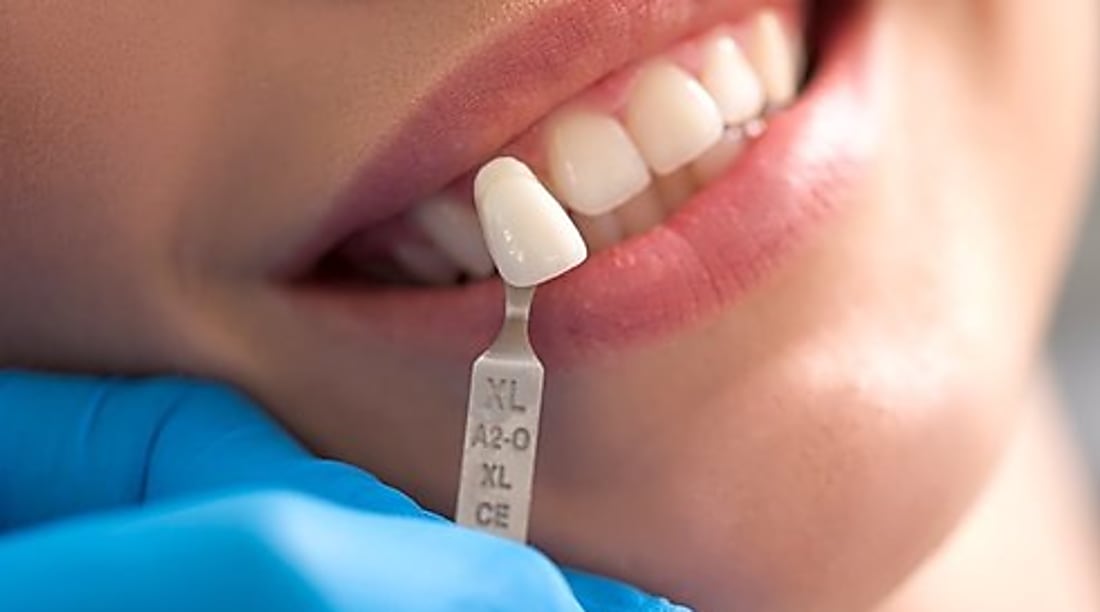
How to apply for dental implants on the NHS
Applying for dental implants through the NHS requires meeting strict clinical criteria and following a defined referral process. Understanding how assessments are conducted, what medical conditions are considered, and which documentation may be needed helps applicants prepare effectively. This guide explains each step of the application pathway, from initial consultation through specialist evaluation, along with expected waiting times and the role of NHS funding decisions. Alternatives available if NHS treatment is declined are also outlined, giving seniors a clearer overview of their options.
Applying for dental implants through the NHS is not a self-referral process and is only available in limited, clinically justified circumstances. The route typically starts with an NHS dentist who evaluates your oral health, considers whether conventional treatments are suitable, and decides if a specialist referral is appropriate. Knowing the criteria, steps, and documents involved will help you prepare and avoid delays.
This article is for informational purposes only and should not be considered medical advice. Please consult a qualified healthcare professional for personalized guidance and treatment.
Key NHS criteria to meet before applying for dental implants
NHS-funded implant treatment is reserved for cases where there is a clear clinical need that cannot be met by conventional options such as dentures or bridges. Circumstances can include tooth loss due to major trauma, head and neck cancer treatment, congenital absence of teeth, severe facial or jaw defects, or medical/anatomical reasons that make dentures unwearable. Good oral and general health are essential: stable gums, controlled decay, excellent oral hygiene, and well-managed conditions like diabetes. Many services also expect smoking cessation, as tobacco significantly increases complications and failure risk. Meeting these criteria does not guarantee approval, but it is a prerequisite for referral and consideration by specialist teams.
What happens during NHS assessments and specialist consultations
If your NHS dentist believes you may qualify, they will submit a referral to a consultant-led service, usually in a hospital-based restorative dentistry clinic. At assessment, the team reviews your dental history, examines the gums and remaining teeth, and evaluates your bite and jaw function. They may request radiographs or advanced imaging to assess bone quantity and quality. You will discuss potential benefits, alternatives, maintenance responsibilities, and long-term risks. The team may recommend preparatory care—periodontal treatment, caries stabilization, hygiene coaching, or smoking cessation—before any decision on implants. In some areas, cases are reviewed by a multidisciplinary panel to ensure fair, consistent application of NHS criteria.
Understanding referral steps and typical NHS waiting times
The process begins with an appointment at an NHS dentist. If you are not currently registered, search for local services in your area using official directories and contact practices directly to ask about availability. Your dentist will explore conventional options first; if these are unsuitable and you meet key criteria, the dentist submits a structured referral with supporting evidence. After triage, you may receive an invitation for hospital assessment. Waiting times vary widely by region and service capacity; in some areas, assessment and treatment stages can take many months and may extend beyond a year. Keeping your contact details updated, attending all appointments, and completing any preparatory treatment can help prevent administrative delays.
Options available if NHS funding is not approved
If the specialist team or funding panel decides you do not meet the criteria, you still have viable paths. Conventional treatments include well-fitted removable dentures or adhesive and conventional bridges, which can restore function and appearance without surgical placement. You might seek a second clinical opinion from another NHS dentist regarding conventional options. University dental schools sometimes offer treatment as part of supervised training; while places are limited and not guaranteed, this can provide an alternative route for complex care. Private treatment is also available outside the NHS, and discussing staged plans, maintenance needs, and aftercare with a qualified clinician can clarify suitability. Charitable organisations may help with urgent dental needs, though they rarely fund this type of treatment.
Preparing documents and information needed for a successful NHS application
Well-organised information makes referrals stronger and assessments smoother. Bring a complete medical history, a list of current medications, and allergy details. Evidence related to your case—such as hospital letters for cancer or trauma, reports from relevant specialists, and previous dental records or radiographs—helps establish clinical need. Photographs (if available), a timeline of events, and letters from other healthcare providers can be useful. Be prepared to demonstrate stable oral hygiene, including completion of any recommended periodontal care. If you have difficulty wearing dentures, describe the problems clearly and bring any existing appliances. While financial status does not determine approval, having proof of exemption for standard NHS dental charges may be relevant for other aspects of care.
Practical tips to stay on track
- Maintain excellent daily oral hygiene and attend routine check-ups while waiting.
- Complete all recommended stabilisation treatments; implant care is long term and requires commitment.
- If you smoke, seek support to stop and document your progress.
- Keep copies of correspondence, imaging, and referrals; bring them to each appointment.
- If circumstances change (health status, medications, symptoms), inform your dental team promptly.
Conclusion Applying for implant treatment on the NHS means demonstrating clear medical necessity, meeting strict clinical criteria, and proceeding through a structured referral and assessment pathway. Being prepared with thorough documentation, stable oral health, and an understanding of possible alternatives can improve your experience, whether or not funding is ultimately approved.