Dental Implants Information for Americans in 2026
In 2026, dental implants remain a popular solution for replacing missing teeth in the United States. Acting as artificial tooth roots, they support permanent or removable teeth and restore oral function. This overview covers key facts about procedures, suitability, costs, and considerations for American patients.
For many U.S. patients, implants are discussed alongside other tooth-replacement options such as bridges and removable dentures. The right choice depends on overall health, gum and bone condition, the location of the missing tooth, and personal priorities like cleaning routines and whether you want a removable or fixed restoration.
This article is for informational purposes only and should not be considered medical advice. Please consult a qualified healthcare professional for personalized guidance and treatment.
Overview of dental implants
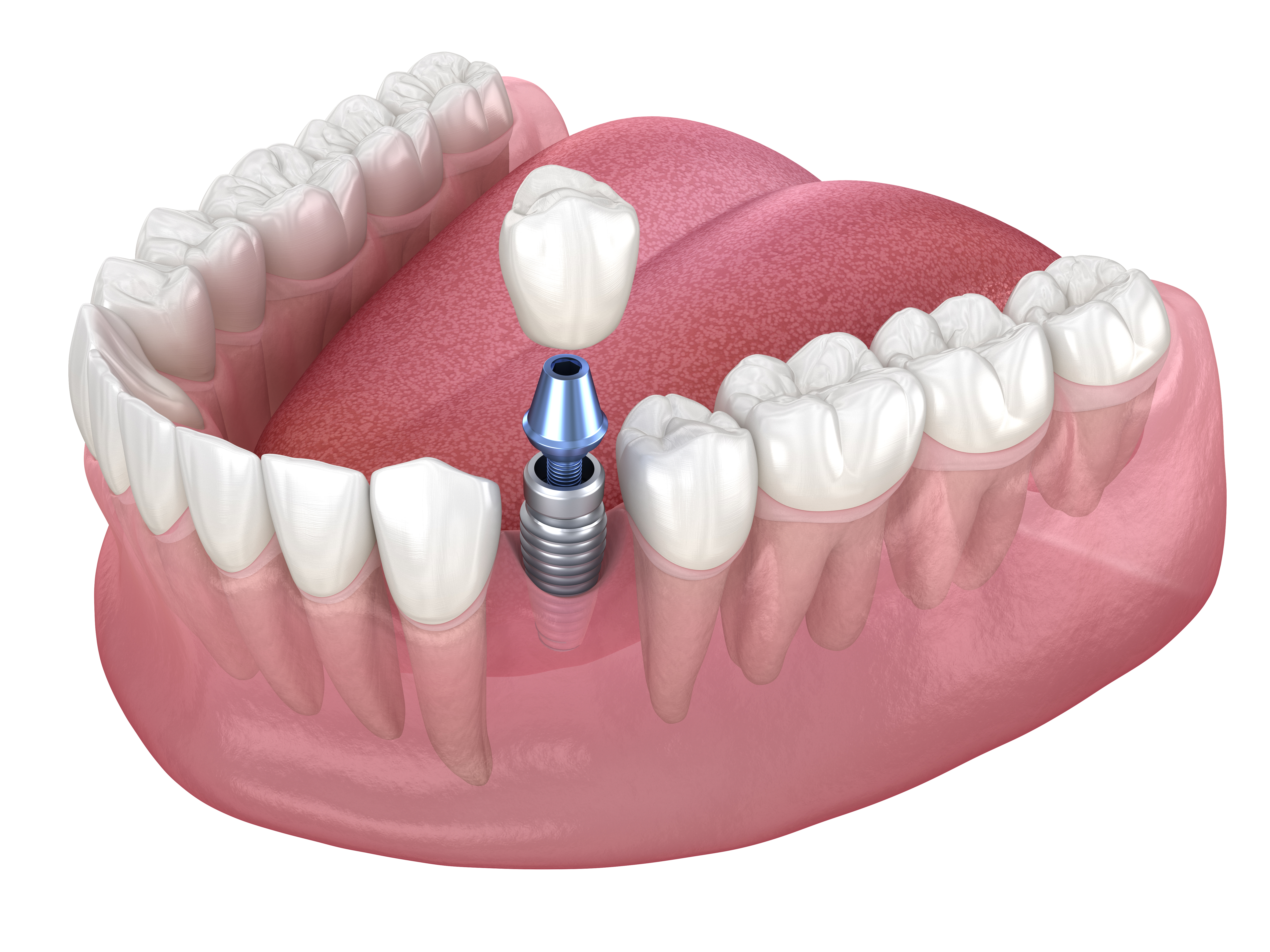
An implant is typically a small post placed in the jawbone that acts like an artificial tooth root. After healing, it supports a connector piece (often called an abutment) and a crown that becomes the visible “tooth.” The most common implant materials used in the U.S. are titanium and zirconia, and the crown may be made from ceramic or other tooth-colored materials chosen for strength and appearance. While implants can be used to replace a single tooth, they can also help stabilize larger restorations, such as implant-supported bridges or dentures.
Implant procedure in the United States: what to expect
The implant procedure in the United States usually follows a staged plan designed to balance safety, healing, and predictable outcomes. Many dental offices use digital X-rays and 3D imaging (such as cone-beam CT) to evaluate bone volume and map nerves and sinuses before surgery. Depending on your case, the plan may include tooth removal, bone grafting, or gum-tissue procedures before or during implant placement. Some patients receive a temporary tooth or temporary denture during healing, while others may go without a tooth in less visible areas until the final crown is ready.
Initial assessment: exams, imaging, and planning
The initial assessment often includes a review of medical history, a clinical exam of gums and bite, and imaging to measure bone and identify anatomical structures. Your dentist may discuss risk factors that can influence healing, such as smoking, uncontrolled diabetes, active gum disease, teeth grinding, or certain medications that affect bone metabolism. Planning also covers practical details: whether you need a bone graft, how many appointments are typical, and what the hygiene routine will look like afterward. This phase is also where shade matching and cosmetic goals are discussed for front teeth.
Surgical placement: how the implant is inserted
Surgical placement generally involves numbing the area with local anesthesia; some practices may also offer sedation options depending on patient needs and the complexity of the case. The clinician creates a small opening in the gum, prepares the bone site with specialized drills, and places the implant to a planned depth and angle. The gum is then closed over the implant or shaped around a healing cap, depending on the approach. Post-operative instructions commonly focus on managing swelling, keeping the site clean, eating softer foods for a short period, and watching for signs that require follow-up.
Healing and integration: timeline, comfort, and aftercare
Healing and integration (often called osseointegration) is the period when bone grows tightly around the implant surface, creating a stable foundation. Timelines vary widely based on bone quality, location in the mouth, whether grafting was needed, and individual health factors. During healing, you may have several check-ins, and your dental team may adjust a temporary tooth to avoid excess pressure on the area. Long-term success also depends on daily cleaning and regular professional care; implants can develop inflammation and bone loss if plaque is not controlled, similar to gum disease around natural teeth.
Choosing providers and understanding common safeguards
In the U.S., implant care may be provided by general dentists with implant training, periodontists (gum and implant specialists), or oral and maxillofacial surgeons, often in coordination with a restorative dentist who makes the crown. It is reasonable to ask who is performing each step, what imaging is used, how complications are handled, and what maintenance schedule is recommended. Written treatment plans typically outline the sequence of procedures and which parts are handled by which clinician. Asking about sterilization standards, emergency availability, and the expected life cycle of crowns or components can also help clarify what “long-term maintenance” means in real life.
Implants are not the only option, and not every patient is an ideal candidate right away. In some cases, treating gum disease, improving home care, or completing grafting and healing first can improve outcomes.
A clear understanding of the steps—assessment, surgical placement, and healing—helps you evaluate benefits and limitations without relying on assumptions. If you are considering implants in 2026, focus on individualized planning, realistic timelines, and consistent aftercare, since long-term stability depends as much on maintenance and health factors as it does on the procedure itself.




