Comparison: Traditional Implants vs. Screwless Implants
Dental implants have revolutionized restorative dentistry, providing durable solutions for replacing lost teeth. In recent years, a new technology has emerged: screwless implants. These promise to simplify the placement process and improve patient experience. This innovation marks a significant advancement over traditional methods, generating interest among professionals and patients alike who seek less invasive alternatives. With many options available, understanding the differences between screwless and traditional implants is crucial for making informed decisions in 2026.
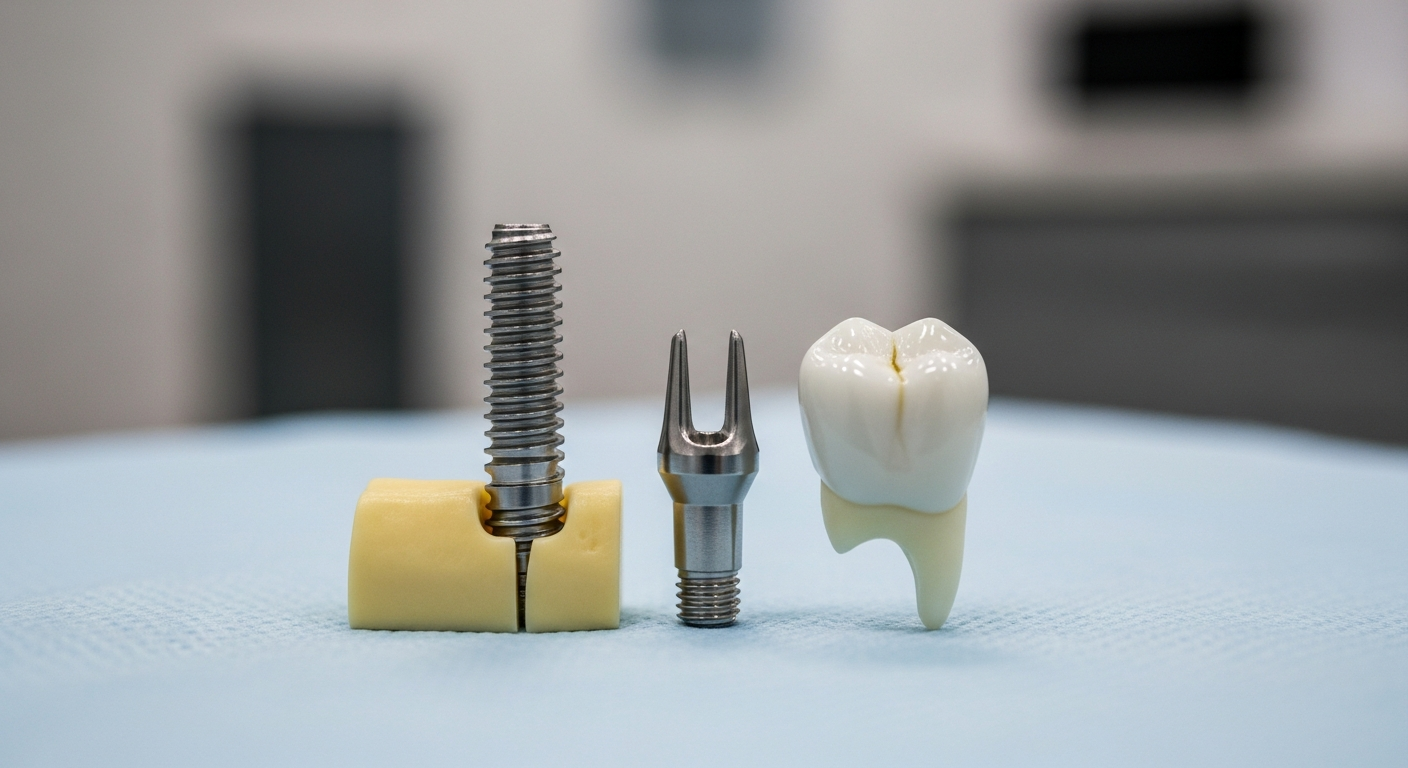
Implant treatment can restore function and appearance after tooth loss, but the details often come down to the connection between the implant, the abutment, and the final crown. “Traditional” options frequently use a small screw to retain components, while “screwless” is a common shorthand for systems that rely on a friction-fit, locking-taper connection. Understanding these terms helps you have a clearer conversation with your clinician about maintenance, retrievability, and long-term planning.
What are screwless dental implants?
In everyday conversation, screwless dental implants usually refer to implant systems where the abutment is retained without an abutment screw, often using a locking-taper (also called a cone or Morse-taper) connection. The implant fixture is still placed surgically into the jawbone like other implants. What changes is how the parts above the bone join together. Instead of tightening a screw, the components are seated with a precise friction fit designed to minimize micro-movement and reduce gaps at the interface.
Why are they becoming so popular?
Interest has grown as patients and clinicians focus more on long-term maintenance and the small complications that can happen with complex restorations. Screw-retained restorations can be highly serviceable, but they may involve screw access holes and the possibility—however manageable—of screw loosening over time. Screwless/locking-taper designs are often discussed because they aim to simplify the emergence profile in certain cases and may reduce concerns about screw mechanics at the abutment level. Popularity also tracks with broader trends: more full-arch reconstructions, more digitally planned cases, and more attention to cleanability and soft-tissue stability.
How do they work?
A traditional screw-retained approach typically involves placing an implant, connecting an abutment (or a multi-unit component), and tightening an internal screw to hold parts together. The crown or bridge may be screw-retained directly or cemented onto an abutment.
With a locking-taper “screwless” approach, the connection relies on precision machining: a tapered post seats into a matching tapered space, creating a friction lock. In practice, the clinician uses controlled force to seat components and specialized tools to retrieve them if needed. As with any implant design, success depends on surgical placement, bone quality, bite forces, hygiene, and a restoration that fits properly.
Comparison between screwless and traditional ones
From a patient perspective, both approaches can support natural-looking crowns and bridges, and both require the same fundamentals: adequate bone, healthy gums, and a stable bite. The differences show up in maintenance style and how repairs are handled.
Traditional screw-retained designs are often valued for straightforward retrievability: if a crown needs to be removed, the screw access pathway can make it more direct. Cement-retained traditional restorations can look seamless but may require careful cement control.
Screwless/locking-taper designs emphasize the integrity of the friction-fit connection. They may reduce the role of screws at the abutment level, but they can require system-specific instruments and clinician familiarity for retrieval and servicing. Neither design eliminates the need for follow-ups, professional cleanings, and monitoring for issues like inflammation, wear, or changes in bite.
Real-world cost and pricing insights (United States) In the U.S., patient pricing usually reflects the full scope of care—consultation, imaging, surgery, the implant parts, and the final crown or bridge—more than whether the connection is screw-retained or locking-taper. A common ballpark for a single tooth replacement (implant, abutment, and crown) is often in the roughly $3,000 to $6,000+ range per tooth, while full-arch fixed solutions can land in the tens of thousands per arch depending on complexity, sedation, grafting needs, and materials. “Screwless” options may be priced similarly because chair time, planning, and restorative work typically drive totals; the biggest cost swings often come from grafting, number of implants, and prosthetic type rather than the presence of an abutment screw.
| Product/Service | Provider | Cost Estimation |
|---|---|---|
| Implant consultation and imaging | Aspen Dental | Varies by location and imaging type; commonly a few hundred dollars without insurance |
| Single-tooth implant with crown (package pricing varies) | Affordable Dentures & Implants | Often quoted in the several-thousand-dollars range per tooth; complexity can raise totals |
| Full-arch fixed implant solution (center-based care model) | ClearChoice Dental Implant Centers | Commonly in the tens-of-thousands per arch; sedation, grafting, and materials can change totals |
| Implant components and restorative materials (clinical supply side) | Straumann / Nobel Biocare / Zimmer Biomet | Patient pricing is indirect; component costs vary by clinic contracts and selected parts |
Prices, rates, or cost estimates mentioned in this article are based on the latest available information but may change over time. Independent research is advised before making financial decisions.
Main benefits of screwless dental implants
The potential benefits most often discussed include a secure, precision-fit connection and reduced reliance on screw mechanics at the abutment level. Some clinicians also prefer the way certain locking-taper systems manage the implant–abutment interface, which can be relevant when trying to support stable gum contours and simplify specific restorative designs.
That said, benefits are case-dependent. A major practical question is serviceability: how easily can the restoration be removed, adjusted, and re-seated over years? In experienced hands, both traditional and locking-taper approaches can be maintained predictably. The “best fit” usually depends on your bite, the tooth position, the planned crown/bridge type, your hygiene routine, and your clinician’s familiarity with the implant system.
This article is for informational purposes only and should not be considered medical advice. Please consult a qualified healthcare professional for personalized guidance and treatment.




