Causes of Daytime Fatigue in Seniors in the United States in 2025
Did you know that changes in sleep patterns and common disorders cause daytime fatigue in many seniors? Understanding these causes—from insomnia to medication effects—can help improve alertness, daily functioning, and overall well-being in older adults.
How Aging Changes Sleep and Contributes to Fatigue
As people age, their sleep architecture undergoes changes. Older adults often experience:
- Earlier bedtimes and wake times
- Reduced total sleep duration, often less than the 7–9 hours recommended for adults
- Lighter, more fragmented sleep with more frequent awakenings at night
- Decreased time in restorative sleep stages, including both REM (rapid eye movement) and non-REM sleep
These age-related changes can disrupt restorative sleep, which is important for daytime alertness and cognitive function. The combined effect may increase feelings of sleepiness or fatigue during the day, even with sufficient time spent in bed.
Factors influencing these changes include shifts in the body’s circadian rhythm and variations in sleep-regulating hormones such as melatonin and chemicals like adenosine. Additionally, older adults may experience a reduced sleep drive, which can contribute to poorer sleep quality and daytime tiredness.
Sleep Disorders and Their Role in Daytime Fatigue
Several sleep disorders are common among seniors and may contribute to daytime fatigue:
Insomnia
- Affects a substantial portion of adults over 60
- Characterized by difficulty falling asleep or staying asleep at least three nights per week
- Can be short-term (due to stress or routine changes) or chronic (lasting longer than three months without an identifiable medical cause)
- May lead to nonrestorative sleep and increased daytime sleepiness
Obstructive Sleep Apnea (OSA)
- Occurs frequently among seniors, with prevalence estimates ranging between 30% and 60%
- Caused by repeated airway blockages during sleep due to relaxation of throat muscles, resulting in breathing pauses
- Leads to fragmented sleep and intermittent decreases in oxygen levels
- Symptoms can include loud snoring, daytime tiredness, memory difficulties, and increased fall risk
- Untreated OSA may be associated with higher risks of heart disease, stroke, diabetes, and cognitive decline
- Diagnosis typically involves polysomnography (sleep studies) performed in a clinical setting or at home
Movement Disorders
- Restless Legs Syndrome (RLS) causes uncomfortable sensations in the legs, prompting movement, especially at night
- Periodic Limb Movement Disorder (PLMD) involves involuntary leg jerks or kicks during sleep
- Both conditions can disrupt sleep continuity and contribute to fatigue
- REM Sleep Behavior Disorder involves the absence of typical muscle paralysis during REM sleep, allowing physical acting out of dreams, further fragmenting sleep and potentially leading to safety concerns
Treatment for these disorders generally involves medical evaluation and may include behavioral therapy, medications, or devices such as CPAP machines for sleep apnea.
Chronic Medical Conditions and Medication Effects
Many older adults have chronic illnesses that can affect sleep quality or cause daytime sleepiness. These include:
- Cardiovascular conditions like heart failure
- Neurological disorders, including Parkinson’s disease and cerebrovascular disease
- Dementia and Alzheimer’s disease, which can disrupt sleep-wake cycles, cause nighttime awakenings, confusion, and daytime drowsiness
- Chronic pain conditions that may interfere with sleep initiation and maintenance
Additionally, medications commonly prescribed for these conditions—such as sedatives, antihypertensives, or antidepressants—may have side effects including sedation, sleep fragmentation, or changes to sleep architecture, contributing to daytime fatigue.
A medical assessment can help in reviewing medication regimens to identify and address potential contributors to drowsiness.
Sleep Changes Related to Dementia and Alzheimer’s Disease
Cognitive decline associated with dementia disorders often affects sleep patterns in several ways:
- Increased daytime napping and nighttime wakefulness or wandering
- Sleep disruptions that may exacerbate memory and cognitive challenges
- Caregivers may also experience fatigue due to increased care demands at night
- Management strategies often focus on improving sleep hygiene, ensuring safety, and addressing coexisting sleep disorders
Lifestyle and Behavioral Factors Affecting Daytime Sleepiness
Lifestyle choices can significantly influence sleepiness during the day:
- Irregular sleep schedules can disrupt circadian rhythms
- Poor sleep hygiene, such as exposure to light or screens before bedtime, may delay sleep onset
- Excessive daytime napping can fragment sleep-wake cycles and interfere with nighttime sleep
- Alcohol consumption near bedtime can reduce sleep quality by causing fragmentation and increasing breathing problems
- Physical inactivity may decrease sleep drive and overall energy
Behavioral interventions, including cognitive behavioral therapy for insomnia (CBT-I), may help improve sleep routines, promote stimulus control, and reduce reliance on medications, which may carry risks in older adults.
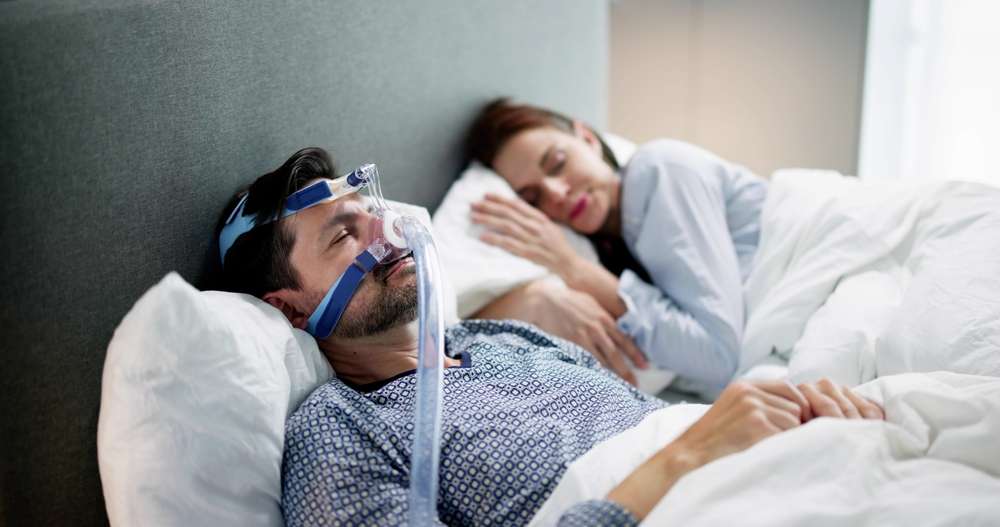
Approaches to Managing Sleep Apnea and Home Environment Adjustments
Sleep apnea is an important factor in fatigue among older adults. Management strategies include:
- Use of Continuous Positive Airway Pressure (CPAP) or bilevel positive airway pressure (BiPAP) devices to maintain open airways during sleep
- Oral appliances designed to reposition the jaw and reduce airway collapse in mild to moderate cases
- Lifestyle changes such as weight management and avoiding alcohol or sedative medications near bedtime
- Adjusting sleeping position, for example, favoring side sleeping
- Modifications at home, including elevating the head of the bed, using humidifiers, and reducing allergens
Following these measures can help improve oxygen levels and sleep quality, which may lead to reduced daytime tiredness and support cognitive function.
Professional Evaluation and Diagnosis Are Important
Persistent daytime fatigue should be discussed with a healthcare provider. Medical professionals can:
- Arrange or perform sleep studies (such as polysomnography or home testing) to diagnose sleep apnea, movement disorders, or other conditions
- Review medication and medical history to identify factors contributing to fatigue
- Recommend suitable treatments ranging from lifestyle modifications and behavioral therapies to the use of medical devices or surgical options when appropriate
Early identification and intervention are important, as untreated fatigue and sleep disorders in seniors may be associated with increased risks of falls, accidents, worsening chronic diseases, and cognitive decline.
In summary, daytime fatigue in seniors in the United States in 2025 is influenced by age-related changes in sleep, common sleep disorders (including insomnia and sleep apnea), chronic medical conditions, medications, dementia-related sleep disruptions, and lifestyle factors. Addressing these factors through individualized approaches involving medical evaluation, behavioral strategies, and appropriate therapies may support improved daytime alertness and quality of life in older adults.
Sources
-
[Sleep and Older Adults National Institute on Aging (NIA)](https://www.nia.nih.gov/health/sleep/sleep-and-older-adults) -
[Excessive Sleepiness in Older Adults: Causes and Solutions OlderAdultCare](https://olderadultcare.com/excessive-sleep-in-elderly/) -
[Addressing Sleep Apnea in Seniors: Signs, Treatments, and Home Adjustments Advanced Care](https://advancedcare.health/addressing-sleep-apnea-in-seniors-signs-treatments-and-home-adjustments-2/)
Disclaimer: All content, including text, graphics, images and information, contained on or available through this web site is for general information purposes only. The information and materials contained in these pages and the terms, conditions and descriptions that appear, are subject to change without notice.